Implant care: prevention and treatment of Peri-implantitis
Several patients suffer from inflammation around dental implants called peri-implantitis. Oxygen-rich BlueM products will offer you a remedy to treat Peri-implantitis effectively!
Peri-implantitis
Peri-implantitis is an infectious disease that causes inflammation of the gum and bone around a dental implant. Chronic inflammation causes bone loss, which can lead to a loose implant that eventually could fall out. The chance of inflammation and peri-implantitis is much higher with implants in comparison to natural teeth, as the implants are not able to attach to the gums as effectively. If the gums are loose around the implants, harmful bacteria can grow below the gums causing bone loss.
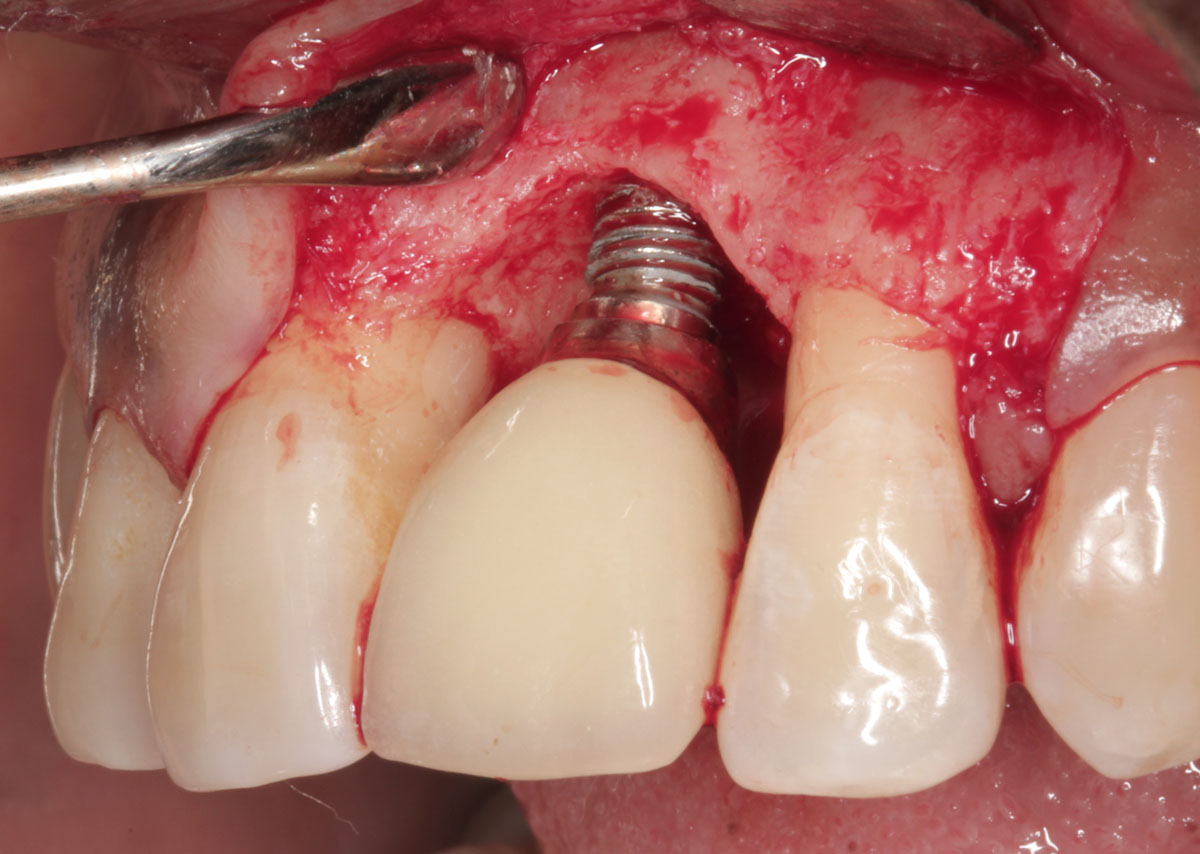
Vision Dr. Peter Blijdorp on peri-implantitis
Anaerobic bacteria
An anaerobic organism or anaerobe is any organism that does not require oxygen for growth. It may react negatively or even die if oxygen is present.Periodontitis and peri-implantitis are thought to be caused by anaerobic bacteria living within the biofilm localized to the subgingival region. Recent investigations of bacterial species associated with periodontitis suggest that the disease is caused by a number of different bacteria and that many novel species may be involved in its etiology.
Advantages of using BlueM products
The oxygen-rich BlueM products can prevent peri-implantantitis. BlueM oral care products:
-
Eliminate harmful bacteria
-
Prevent and repair infections
-
Penetrate deep into the pockets
- Contribute to the stimulation of bone growth
In addition, BlueM products are fluoride-free. Although fluoride has many benefits, it corrodes the titanium layer of the implant. BlueM toothpaste, mouthwash and oral gel don’t contain fluoride, reducing the risk of loosing an implant.
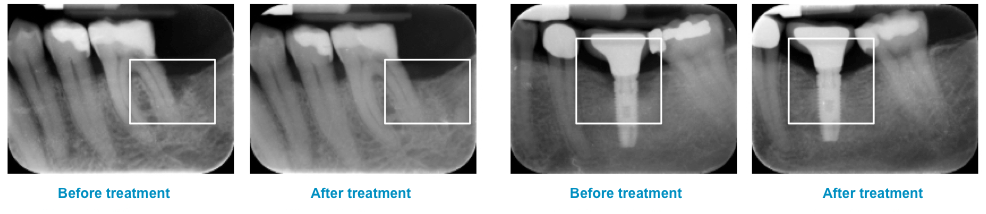
Below are the results of treating peri-implantitis with the BlueM oral gel: The marked area significantly shows bone growth.
BlueM peri-implantitis treatment
To prevent or treat peri-implantitis, Dr. Peter Blijdorp recommends to brush twice a day with BlueM toothpaste and to rinse twice a day with BlueM mouthwash. Subsequently, apply the BlueM oral gel one or two times a day underneath the implant or where it is needed and leave the gel as long as possible on site. Use the Terumo syringes to apply the gel on the hard-to-reach areas in the mouth. Visit your dental professional and ask for BlueM to treat Peri-implantitis!
Peri-implantitis: The ‘time bomb’ in dental implants
By Ruth Wood (Telegraph Media Group)
A little-known disease is emerging in which bacterial infection causes the loss of the bone supporting the implant.
Cathy Gunnell was thrilled when she had dental implants fitted at the age of 52. Since childhood, she’d endured crooked teeth, gum disease and abscesses, one of which forced her to have a tooth removed. So when a local London clinic charged her £13,000 to replace four diseased teeth with gleaming white porcelain ones, fixed in place with metal pegs, she was more than happy to pay. That was in 2002, and for 12 years she had no problems. But three months ago, she felt a lump on her lower right jaw near one implant. “There was no pain, but I got it checked out by my local dentist,” says Mrs Gunnell, now 64. The lump was caused by inflammation that cleared up after antibiotics. But an X-ray showed the bone supporting the implant was receding. To her shock, Mrs Gunnell’s dentist diagnosed her with a little-known disease that is now emerging as a serious complication of dental implants. It is called peri-implantitis, and has been described as a “time bomb” by a leading dental surgeon.
Peri-implantitis is an inflammatory disease marked by bacterial infection and the gradual loss of the jaw bone supporting the implant. It’s not yet clear whether the infection causes the bone to recede, or the bone loss exposes the area to bacteria. Dentists are uncertain how to treat it. “I was shocked,” says Mrs Gunnell. “I’d never heard of the disease.”
Ten years ago, professionals said the condition didn’t exist. But now it is on the rise, as increasing numbers of people have replacement porcelain crowns with titanium roots. Half-a-million adults have at least one dental implant, according to the latest Adult Dental Health Survey. Studies have suggested that one third of patients will be infected. “We’re sitting on a time bomb,” says Dr Stephen Jacobs, a past president of the Association of Dental Implantology and well-respected implant surgeon. “We are going to be seeing more and more cases.” Peri-implantitis is always preceded by a much milder disease, called peri-implant mucositis, which is common and treatable. Early warning signs are red, swollen gums and bleeding when probed. If undetected and untreated, it might become peri-implantitis. Because bone loss is painless, many people don’t realise they have the condition. So scrupulous oral hygiene and regular follow-up appointments after an implant are essential, says Dr Jacobs, who runs a Glasgow clinic. “One of the problems with seeking treatment abroad [as many do in search of cheaper treatment] is the lack of lifelong maintenance and follow-up, which is a key part of the care process.”
Mrs Gunnell stopped going for check-ups three years ago, after she moved from London to Devon. She was at high risk of peri-implantitis because of a family history of gum disease (periodontitis). Smokers, too, are at high risk.
Paradoxically, the rise in cases is mostly due to advances in implant design. In the mid-Nineties, clinicians found that implants with a rough instead of a smooth surface integrated better with the bone. However, the textured surface is more likely to harbour bacteria if the bone shrinks away from it. After her recent diagnosis, Mrs Gunnell returned to the London prosthodontist who originally treated her. “He removed the bridge and screws and deep-cleaned the whole area and all the components,” she says. “He told me to brush with TePe brushes [small interdental brushes] dipped in BlueM oral gel, morning and night, and to come back for yearly check-ups. Hopefully.
Visit your dental professional and ask for BlueM to treat Peri-implantitis!
Study Dr. N.V. Pandya about treating peri-implantitis
Aim of the study: To examine the effectiviness of topical oxygen (BlueM) therapies in a treatment regime for peri-implantitis.

TOOTh advice: Topical Oxygen Therapy with BlueM
Visit your dental professional and ask for BlueM to treat Peri-implantitis!